 After more than 125 years of providing extraordinary care to sick and injured infants, children and teenagers, Floating Hospital for Children, renamed Tufts Children’s Hospital will be closing. “Floating Hospital started as a ship in Boston harbor, back in the day when doctors thought that sick kids needed the clean sea air to get better,” said Geoffrey Binney, MD, Pediatrician-in-Chief at Tufts Children’s Hospital. “It’s a rich history, but unfortunately, even after all this time, the name hasn’t resonated with the people of Boston and surrounding towns. Changing the name to one aligned with the Tufts brand will help us receive attention commensurate with the outstanding pediatric care we have provided for more than a century.” in the past several years, Floating cared for 40,000 children each year. In 1894, its inaugural year sailing Boston harbor, Floating Hospital treated 1,100 children in need. It wasn’t long after that a research facility was built on land to explore new pediatric medical treatments. One such discovery came in 1919 – the first-ever artificial milk product, today known as Similac. In 1927 when a fire destroyed the ship, hospital trustees decided to move all clinical services on shore, as well. In 2016, I knew almost nothing about Boston's Floating Hospital when I began working there in the pediatric hematology/oncology clinic as a massage therapist with Lucy's Love Bus. Six years later, as the pediatric wards close and I walk out the doors one final time, I am both saddened and angered that Boston lost a medical and historical landmark of unprecedented significance - and heartbroken that our Floating Families lost a home. What I've experienced, learned, shared in, and witnessed from our kids, our families, and our most dedicated staff, will remain with me always. “We will always cherish the hospital’s history and its legacy,” said Rachel Wasserstrom, Vice President, Tufts Children’s Hospital, Women’s Health and Psychiatry. “It has been an unbelievable 125 years caring for everything from stomach aches to the most complex medical conditions...."
0 Comments
by Virginia Murphy
Here is a quick follow-up to my original blog post on Post Surgery MLD, which can be found here I wanted to share with you my thoughts about lymphatic drainage after liposuction/BBL (Brazilian Butt Lift). I have had so many calls about it since September and I have worked on a few patients that had these surgeries and most of them told me that my work was not similar to what they received in Florida. My only answer is, they didn’t receive MLD. I am certified Lymphedema Therapist, trained in the Vodder Method. Because I am also an oncology massage therapist, I am able to treat lymphedema - and manual lymphatic drainage is the only recommended treatment for that. Manual lymphatic drainage can also be considered for post operative surgical swelling due to liposuction. Many of these surgeries seem to be happening in Florida. Some clients who have called have indicated that the MLD treatments they received there were painful. Done properly, MLD is very gentle and it doesn't hurt. However, there is little to no clinical evidence that it will speed up the healing process or decrease scar tissue/fibrosis. What it can do is move the swelling/edema and help you relax. The healing process is natural and normal and your body knows what it needs to do. Helping you through it, is where MLD is useful. I love my work and I’m dedicated to positive outcomes. I am also very transparent with my patients and want to create realistic expectations. There is much misunderstanding surrounding this topic, like many massage related topics. Your body, having been subjected to surgical trauma, needs to heal. Inflammation is a natural part of that process, as is pain, sorry to say. In my opinion, it is not a good idea to try and circumvent the bodies natural healing process, but rather, what I prefer to do is assist it and you by helping move accumulated fluids and help your body relax, which will in turn make the healing process less painful. Massage is incredibly useful and beneficial but it has limitations. If you have had experiences with post surgical MLD or thoughts, please add them to the comment below. In the meantime, if you are contemplating an elective procedure or have just gone through surgery and would like to book an appointment or request a consultation, please email me here. Manual Lymphatic Drainage after Liposuction
by Virginia Murphy Because I’ve had so many people reach out to me about manual lymphatic drainage (MLD) after cosmetic surgeries such as Liposuction, I feel it necessary to share an article which parallels my thoughts on this. MLD is a manual technique that helps promote the movement of fluid (lymph) out of a swollen area of the body. It is extremely gentle and incredibly relaxing. And yes, MLD does assist with post operative swelling, however there is not enough evidence supporting its other claims. The information which has been shared with me and what I have discovered, is that what’s being offered after these surgeries is anything but gentle and is quite possibly not necessarily helpful. If you’re interested in discussing, please email me. MANUAL LYMPHATIC DRAINAGE AFTER LIPOSUCTION By: Ryan Davey, PhD Manual lymphatic drainage (MLD) massage is frequently recommended by plastic surgeons during the recovery phase following cosmetic liposuction. This specialized form of massage is generally believed to decrease recovery time and improve results, by reducing post-surgical swelling and fibrosis (scar tissue formation). But is manual lymphatic drainage after liposuction really warranted? If so, for which patients? LIPOSUCTION CAUSES SWELLING AND TISSUES DAMAGE THAT NEEDS TO BE MANAGED FOR BEST RESULTS During the early period following liposuction surgery patients will experience swelling, bruising and discomfort. This is to be expected since liposuction is a relatively invasive procedure. Common forms of liposuction involve either injecting a significant amount of medicated fluid into the area (‘tumescent’ or ‘super wet’ techniques) or using ultrasonic vibration or laser to liquefy the fat, before suctioning it out using a sharp-ended vacuum tube (a ‘cannula’). These procedures can create significant tissue damage. SOME SIDE-EFFECTS OF LIPOSUCTION ARE EXPERIENCED BY EVERY PATIENT - AND SHOULD BE MANAGED BY EVERY PATIENT The popular opinion of fat is that it’s simply an undesirable lumpy white mass of stored calories, but this is far from the truth. Fat is an important and active living tissue. Comprised primarily of adipocyte cells (which store lipids) and connective tissue (the glue that holds tissues together), fat is heavily vascularized (lots of blood vessels and lymphatic vessels) and plays key roles in energy storage and hormonal regulation. Removing fat by liposuction causes damage to blood and lymphatic vessels as well as the destruction of cells and connective tissue. This has the double effect of causing blood and lymph fluids to accumulate, while also creating more space for it to pool. [Interesting side note: The circulatory system (arteries and veins) and the lymphatic system (lymph vessels and nodes) work together to maintain the fluid balance in tissues. Arteries deliver blood to the tissue, a nutrient rich fluid bathes the cells, and then this fluid returns to the circulatory system via the veins, AND via the lymphatics (where it is known as ‘lymph’). Both venous and lymphatic systems need to be functional to maintain an appropriate fluid balance in tissues, and when either fail, swelling results (chronic venous insufficiency or lymphedema, respectively).] Post-surgical pooling of blood and lymph fluid should be monitored for every liposuction patient, and when necessary, treated, as should tissue separation caused by the sweeping action of the suction tube. Without proper management of these side effects poor aesthetic outcomes can result, along with the possibility of longer recovery times, greater pain, and health complications. The abdominal compression garment put on in the operating room and worn thereafter (as per surgeon instructions) accomplishes the dual tasks of decreasing the pooling of blood and lymph (much like applying pressure to a wound stops the bleeding) and bringing the separated tissue in close proximity to encourage healing. Insertion of small drainage tubes into the spaces where fat was removed can further prevent pooling over the first few days following surgery. OTHER SIDE-EFFECTS OF LIPOSUCTION CAN VARY FROM PERSON-TO-PERSON AND SO INDIVIDUAL POST-OPERATIVE NEEDS VARY For some patients, standard interventions will suffice, recovery will be fast, and aesthetic outcomes optimal. Unfortunately, not every patient will have this experience. The post-surgical recovery process varies person-to-person according to a variety of factors including the type and extent of liposuction, age, health and physical activity levels, skin characteristics, smoking, complications such as infection, and so on. Variable side effects include: Scarring Inflammation and repair processes bring immune cells to the area to help clean out dead tissue and waste, and new connective tissue is laid down to help knit the tissue back together. When the accumulation of connective tissue is significant (known as ‘fibrosis’ or scarring) this process thickens the tissue and decreases its pliability. Excessive fibrosis may be felt by hand, may restrict motion or produce feelings of tightness, and may even be visually noticeable. Scarring will naturally diminish with time as the tissue gradually remodels itself, but this process can be long and some scarring is likely to be permanent. Prolonged swelling or swelling pockets In general, swelling may be greater than necessary if compression garments are removed too early, not applied properly or consistently, or not sized appropriately. Excessive fluid presence or localized pockets of fluid may slow recovery and/or make the results less aesthetically optimal by encouraging uneven healing and fibrosis. Uncontrolled swelling could potentially create other complications such as small pockets of fluid becoming trapped (called a ‘seroma’), inflammation, and infection. HOW SHOULD THESE VARIABLE SIDE EFFECTS BE MANAGED? Judicious adherence to your surgeon’s recommendations, including follow-up, is the best way for you to minimize your recovery time, optimize your results, and avoid potential complications. Surgeons often recommend that their patients supplement their recovery with manual lymphatic drainage as early as possible, ideally within the first few days post-surgery. The idea behind this recommendation is that manual lymphatic drainage could potentially help prevent and alleviate the build-up of fluid and formation of scar tissue. But where does this recommendation come from? Some of the surgeons who recommend manual lymphatic drainage also benefit financially from offering it to their patients as an add-on service. So how do we know this is a worthwhile recommendation? SHOULD WE EXPECT MANUAL LYMPHATIC DRAINAGE AFTER LIPOSUCTION TO BE BENEFICIAL? Plastic surgeons frequently recommend manual lymphatic drainage after liposuction, or after abdominoplasty with liposuction (a ‘tummy-tuck’). It’s also recommended as a post-liposuction treatment by the Dr. Vodder School, the largest manual lymphatic drainage massage training and certification body. Nevertheless, why should we expect it to help? WHAT IS MANUAL LYMPHATIC DRAINAGE (MLD) AND WHAT DOES IT DO? Manual lymphatic drainage massage is offered by registered physiotherapists and massage therapists (and other health professionals) who have received additional training and certification. Using sequences of gentle massage strokes, manual lymphatic drainage helps to stimulate the flow of fluid through the lymphatic system, thus relieving swelling. This technique is routinely offered along with compression garments and education as part of Combined Decongestive Therapy (CDT), the standard treatment for patients with chronic lymphatic insufficiency (lymphedema). But should we expect it to help patients recovering from liposuction? SHOULD IT BENEFIT LIPOSUCTION PATIENTS? While many plastic surgeons recommend it, some don’t. I noticed one plastic surgeon commented online that they didn’t believe it was ‘possible’ to manually push fluid through the lymphatic system. They went on to say that many patients describe lymphatic massage to be ‘excruciatingly painful’. Perhaps this could be the case if the technique was performed incorrectly, or by someone who is not certified, but otherwise it is easy to demonstrate that both of these comments are incorrect. Here’s why: Manual lymphatic drainage is a central component of CDT, which is the treatment recommended by the International Society of Lymphology for managing chronic swelling in patients with lymphatic insufficiency (lymphedema). Imaging studies confirm that manual lymphatic drainage massage significantly increases the flow of fluid in lymphatic vessels in normal individuals (ref 2). This finding explains the large number of clinical studies and anecdotal observations collected over decades of use that demonstrate its clinical effectiveness (for a recent systematic review see ref 3). It’s also important to note that pain is not described as a side-effect of manual lymphatic drainage massage in these studies, nor is it mentioned by any knowledgeable publication or web article. To the contrary, manual lymphatic drainage is more gentle than conventional massage and is frequently described as enjoyable. This also coincides with our own experience. But this same surgeon is correct in suggesting that there is likely little to no scientific evidence supporting massage of any type after liposuction. The question isn’t whether manual lymphatic drainage can reduce swelling – it can. The question is whether manual lymphatic drainage after liposuction can offer patients a quantifiable clinical benefit over standard care. Unfortunately, we can’t answer this question with clinical study data; I can find only primarily anecdotal support in the clinical literature rather than proper clinical studies (for example, see ref 4). The jury is still out. There is insufficient evidence to suggest that manual lymphatic drainage should be recommended to all liposuction patients, and I would suspect that it would have little benefit in some patients. But is there a group of liposuction patients we would expect it to benefit? Yes. The available information suggests that manual lymphatic drainage would help relieve swelling in liposuction patients who are having difficulty controlling swelling otherwise, and furthermore, that eliminating excessive swelling would be expected to speed recovery and improve results (such as less fibrosis and improved skin texture). WHAT IS IT LIKE TO RECEIVE MANUAL LYMPHATIC DRAINAGE AFTER LIPOSUCTION? Manual lymphatic drainage is usually delivered in one-hour sessions, and should include some education on self-care practices. It is not painful, much more gentle than regular massage, and is usually described as being pleasant. No oils or other products are used on the skin during these sessions. Surgeons typically recommend for best results that care be initiated in the first few days following surgery (within the first 5 days), and some recommend that patients come for a standard number of treatment sessions. However, the number of sessions should ideally be determined by the therapist in conversation with the patient and based on: the amount of swelling; patient responsiveness to treatment; patient commitment to self-care practices; and of course, on the patient’s perception of benefit and financial considerations. Patients should experience some benefit from the very first treatment, and may find that this benefit increases upon subsequent visits, but typically no more than a handful of sessions are required to achieve maximal benefit. *POSSIBLE* BENEFITS OF MANUAL LYMPHATIC DRAINAGE AFTER LIPOSUCTION
*POSSIBLE* NEGATIVE SIDE EFFECTS OF MANUAL LYMPHATIC DRAINAGE AFTER LIPOSUCTION Manual lymphatic drainage has been shown to be a safe technique with very few complications or contraindications. This includes for patients who have recently undergo breast cancer surgery (a common risk factor for lymphedema). The same holds true for liposuction patients, with the caveat that liposuction patients seen shortly after their procedure have wounds that are actively healing and appropriate care should be taken. WHICH LIPOSUCTION PATIENTS MIGHT BENEFIT MOST FROM MANUAL LYMPHATIC DRAINAGE The patients who stand to benefit most from manual lymphatic drainage would be those with a lot of swelling, and/or with swelling that is difficult to reduce. Typically, these are patients where compression garments couldn’t be used, weren’t used effectively, or weren’t used at all. Liposuction patients that experience fluid build-up away from the surgical site, such as in the legs, could also benefit. With respect to fibrosis, patients with more extensive procedures are more likely to benefit from the fibrosis-reducing effects of manual lymphatic drainage. Other patients may benefit psychologically. Since it is a safe and enjoyable massage technique, it may be beneficial to consider it for patients who might otherwise wonder or worry that their recovery could have been easier, or their results better, or for patients who exhibit fear-based touch-avoidance after this sort of procedure, and who can afford the additional expense. SUMMARY Manual lymphatic drainage post-liposuction is recommended by many plastic surgeons, as well as by the Dr. Vodder School (the largest manual lymphatic training and certification body). But should manual lymphatic drainage be broadly recommended to patients following liposuction? Maybe. Broad recommendations should typically be reserved for treatments where reasonably strong clinical evidence exists, and where the benefits outweigh the risks. For example, manual lymphatic drainage (as part of ‘combined decongestive therapy’) is the recommended treatment for the chronic swelling condition known as lymphedema. Unfortunately, there have been very few clinical studies to examine the benefits and risks related to the use of manual lymphatic drainage after liposuction, so strong clinical evidence does not exist to support a general recommendation. With that said, based on our understanding of manual lymphatic drainage it seems very likely that at least some liposuction patients would stand to benefit from it. And for those who are unsure of the benefit, the experience should still be pleasant and without negative side effects. Read my follow-up to this blog post on Post Surgery MLD, which can be found here References
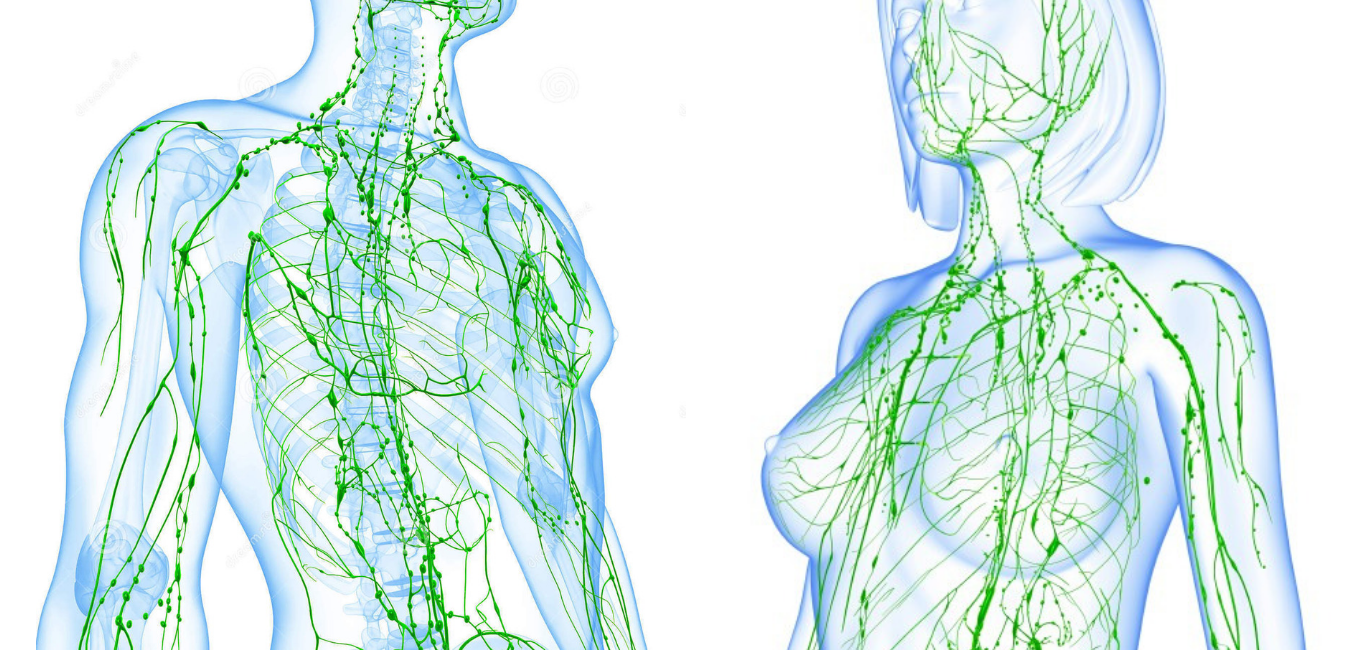
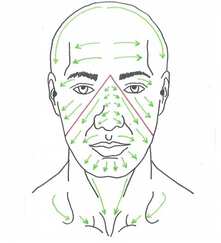 Combating Allergies with MLD by Virginia Murphy Spring is well underway. Pollen is here. Unfortunately, for many people, so are their allergies. This is the season for hay fever, allergic asthma and eczema to have their wicked way, which means sufferers endure a catalogue of unpleasant symptoms. Sneezing, coughing and wheezing, along with itchy eyes, fuzzy heads, runny noses and rashes force many people to rely on antihistamines. What causes allergies anyway… tiny grains of pollen from trees, grasses, crops, weeds etc. become airborne. Once inhaled these irritating invaders enter your respiratory system triggering allergy and asthma symptoms that affect over 50 million people in the US alone. One non-chemical way to help your body rid itself of some of those allergy symptoms is through Manual Lymphatic Drainage of the neck and face. What is the lymphatic system? The lymphatic system is the body’s natural detoxification and drainage network. It helps deliver hormones and nutrients through the body and works closely with our blood circulation, via a framework of vessels linked by lymph nodes and organs such as the spleen. How can MLD help? Developed in the 1920s, manual lymphatic drainage (MLD) is a scientifically proven form of massage therapy that clears congestion caused by a build-up of lymph fluid in the body’s tissues. The gentle technique clears allergens and histamines, and is a great treatment for skin and digestive conditions, glandular fever and many others, soothing and calming the nervous system. Benefits of treatment By promoting good lymph flow, MLD equips the body's defense system to react properly, meaning a strengthened immune system and the ability to deal with allergens better. When one suffers from allergies, the body’s immune system goes into high gear as it overreacts to pollen, mold spores or other foreign body invaders. The result is irritation and inflammation of the sinuses. Lymphatic drainage can help to relieve these symptoms. Consider Booking a Therapeutic Massage with MLD add on to experience it for yourself. By Ginny Murphy
Lymphedema is one of the scariest long term side effects of breast cancer treatment. It can result when lymph nodes are removed or damaged by surgery and/or radiation. Disfiguring, distressing, and often disabling, lymphedema can only be managed and controlled, not cured. Those who have been treated for breast cancer are at risk for developing this condition, and that risk remains life-long.Many doctors don't have a great deal of experience with the diagnosis and treatment of lymphedema because medical schools don't teach the lymphatic system at all. A national survey conducted by Dr. Stanley Rockson, Professor of Lymphatic Research and Medicine, Stanford University, showed that the average time spent on teaching the lymphatic system during a four year medical school education is 15 minutes. Left untreated, lymphedema can worsen and cause severe swelling and permanent changes to the tissues under the skin, such as thickening and scarring.On Friday evening (7/29) will go over the basics of the lymphatic system in order to gain a better understanding of why lymphedema can occur, as well as risk factors and prevention. The last part of the evening will be spent learning self MLD techniques for lymphedema risk/history.Although there is no way to know whether you will develop lymphedema after breast cancer surgery and/or radiation, it is crucial to become educated on risk factors, risk reduction practices, symptoms, and treatment. Remember, knowledge IS power...  By Ginny Murphy For ages, I've been thinking about writing a blog about cancer and integrative therapies. But what was holding me back was trying to figure out what to write about first, since there's so much information I want to share. So here I am - ready to share my passion for oncology massage, which truly feels like my mission. In my blog posts I’ll talk about what originally led me to this work, what happens when one receives a cancer diagnosis, cancer and its side effects, living with cancer, end of life care, care giver support, research supporting oncology massage, and healing versus curing... But where I want to begin is to talk about “healing versus curing." I bear witness to this all the time. I see it at Be Well. I see it with my patients in hospice and I see it with the kids at Tufts Floating Hospital. Let's face it, when one receives a cancer diagnosis, it's a game changer. After the initial shock, when the dust begins to settle, a cure is what one aims for. And because we are at an unprecedented precipice in cancer treatment (i.e. immunotherapy), this is a real possibility in many scenarios. I've seen people cured - or more accurately the term NED (no evidence of disease) is used. Some cancers of the blood are deemed curable, in particular ALL (the most common form of leukemia in children), with a very high survival rate. In the short time I've been working in the pediatric hematology/oncology clinic at Tufts, I see this extraordinary chain of events played out weekly. Surgery, radiation, and chemotherapy - all lifesaving - come at a cost. The stories I hear from my patients and clients all share a similar theme; their bodies are not the same. Yet oncology massage can bring bodies to a place where they move easier due to an increased range of motion, it can soften tissues that are rigid and scarred, and it can decrease pain and help to relive feelings of anxiety. It can indeed begin to change the body. These bodies and minds eventually come to accept this as their new normal...and this can be called "healing." The simple and timeless act of "laying of hands"on another, is for me what this is all about and where the healing occurs. There is something so profoundly sacred in this exchange. It does not need to be proven nor researched. I trust this process and I am beyond fortunate and humbled to call this my work. "Touch was never meant to be a luxury. It is a basic human need. It is an action that validates life and gives hope both to the receiver and the giver." ~ Irene Smith |
Author
I write about topics I am interested in and or passionate about. -Virginia ArchivesCategories
All
|
Proudly powered by Weebly





 RSS Feed
RSS Feed